Tinnitus: Causes and Treatment
 The high-pitched sound at the beginning of the TV show Outer
Limits is very similar to the sounds heard by many tinnitus sufferers.
The high-pitched sound at the beginning of the TV show Outer
Limits is very similar to the sounds heard by many tinnitus sufferers.
 n the United States, about
10-15% of the population suffer from tinnitus, known colloquially as
"ringing in the ears." Tinnitus is not just unwanted noise; it is extremely
unpleasant and often interferes with enjoyment of music. It can make verbal
communication impossible and can cause depression.
n the United States, about
10-15% of the population suffer from tinnitus, known colloquially as
"ringing in the ears." Tinnitus is not just unwanted noise; it is extremely
unpleasant and often interferes with enjoyment of music. It can make verbal
communication impossible and can cause depression.
Conventional medical thinking used to be that tinnitus arises from injury to cells in the inner ear or the vestibulocochlear nerve (also known as the acoustic nerve, auditory nerve, or cranial nerve VIII), and is therefore difficult or impossible to treat. However, it is now recognized that this is not always the case. Researchers now realize that rewiring of an area in the brainstem called the dorsal cochlear nucleus plays an important role in tinnitus. This new understanding of its causes may result in new treatments for many patients. Indeed, recent results based on this theory are already leading to effective forms of treatment in some patients.
However, many physicians are unaware of the causes of tinnitus and the problems endured by tinnitus sufferers, and they will often tell the patient that the problem is imaginary or unimportant. This often causes the patient to abandon attempts to get treatment. This is unfortunate, because recent research suggests that tinnitus is easier to cure when treatment is given early. In this article, I will discuss what is known about tinnitus and what tinnitus sufferers can do about their affliction. The information on this page is not medical advice, but is presented for informational purposes.
Types of tinnitus
One way tinnitus can be classified is by the type of sound. By this criterion, there are three main types of tinnitus:
Continuous ringing or hissing
In this type of tinnitus, the patient hears a continuous, high-pitched
ringing or hissing sound that is unaffected by body movement. Often,
tinnitus is accompanied by a partial loss of hearing. Usually, only higher
frequencies are lost.
Researchers believe it is no coincidence that tinnitus sufferers most often report hearing high-pitched sounds. High frequencies (around 4kHz) are usually the first to be lost after noise trauma (which is a major cause of sensorineural hearing loss), as well as in presbycusis (age-dependent hearing loss). As many as 80% of tinnitus sufferers also have some form of hearing impairment. It is believed that the nervous system adapts to this loss of acoustic stimuli by creating artificial phantom sounds. This is analogous to phantom limb syndrome, where constant pain is felt in a limb after it has been amputated. Thus, patients with a history of exposure to loud noise are most likely to report hearing high pitched ringing sounds.
The pitch of tinnitus often coincides with the frequency region in which the audiogram starts to show a steep decline. This suggests that tinnitus might result from an "edge effect" caused by the brain's attempts to equalize different parts of the acoustic spectrum [16].
There is some relationship between pitch and cause of tinnitus. In the ear, higher-pitched sounds are detected in the outermost portion of the cochlea. Thus, the frequency may depend on the exact part of the inner ear where the original injury occurred. Tinnitus caused by sensorineural hearing loss is usually high pitched. The tinnitus that occurs in Ménière's disease, a disease of the inner ear, is typically of a much lower pitch.
| Cause | Median frequency, Hz | Frequency range |
|---|---|---|
| Sensorineural hearing loss or Otosclerosis |
3900 | 545-7500 |
| Conductive hearing loss | 490 | 90-1450 |
| Meniere's Disease | 320 | 90-900 |
Ringing affected by body position
When the ringing sound is made better or worse by changes in body or
neck position, it is called somatic tinnitus. This is the most common
type of tinnitus.
Non-ringing
When the sound is not a ringing, but a rushing, clicking, thumping, or
other atonal sound, it usually represents some mechanical process in or
near the ear. Often these sounds can be heard by another person using a
stethoscope, and therefore they are called "objective" tinnitus. A
common example is a pulsatile bruit caused by turbulent flow through blood
vessels in the neck.
Clicking sounds are often associated with temporomandibular joint (TMJ) syndrome. Clicking sounds can also be caused by intermittent contraction of various muscles in the middle ear, including the tensor tympani or stapedius muscles. This condition is called middle ear myoclonus. Although thought to be rare, it may actually just be widely undiagnosed. A related condition is palatal myoclonus. A physician may prescribe muscle relaxants such as orphenadrine, or in severe cases, may inject botulinum toxin to stop the muscle from contracting.
Another way to classify tinnitus is between bilateral and unilateral tinnitus. Treatment is different for each type. For example, microvascular decompression (see below) is usually ineffective against bilateral tinnitus.
Causes of tinnitus
In general, tinnitus usually starts with some injury to the ear--either a noise trauma, a blow to the head, or some disease-induced injury. According to the current theory, a part of the brainstem called the dorsal cochlear nucleus tries to adapt to the injury, but in so doing creates phantom sounds. Some of the causes of tinnitus can be very serious, and indicative of some underlying pathology, while the majority of cases are much less serious.
Pathological causes
Pathological causes of tinnitus include head injury; disorders affecting the CNS such as stroke, meningitis, and encephalitis; cardiovascular disorders such intracranial hypertension, aneurysm, aortic stenosis, or carotid artery stenosis; ear infections, cancer, and surgery-induced injury.
Tinnitus is always present in a type of cancer known as vestibular Schwannoma, and is usually present in acoustic neuroma. Tinnitus, along with vestibular (balance) problems, is always present in Ménière's disease, a serious disorder of the fluid balance mechanism of the inner ear. Other possible causes are vascular tumors or large arteriovenous malformations.
Lermoyez syndrome is an acute condition similar to Ménière's disease characterized by tinnitus, hearing fluctuations, and vertigo. Unlike Ménière's disease, it is not considered to be progressive but strikes at a younger age. Like Ménière's disease, Lermoyez syndrome is caused by increased hydraulic pressure in the inner ear (endolymphatic hydrops). The patient experiences an elevation of low-frequency hearing threshold that progressively worsens for a few days to months preceding an acute attack. After the attack, which lasts for several hours, hearing improves.
Injury to the auditory nerve (8th cranial nerve) produced by certain types of surgery produces gaze-induced tinnitus, in which the intensity of the sound changes when the patient changes the angle of their gaze.
Hyperthyroidism, as in conditions like Graves' disease, is another possible cause of tinnitus. The opposite condition, hypothyroidism, frequently causes tinnitus as well as hearing loss. Thyroid patients need to have their thyroid hormone levels monitored periodically to avoid losing their hearing.
Tinnitus is sometimes present in Wilson's disease, an inherited condition in which copper accumulates in the liver.
Another cause of hearing loss and tinnitus is Paget's disease of bone, which is a disorder caused by increased bone turnover and enlarged areas at discrete areas of the skeleton. Paget's disease has a genetic (familial) component and occurs more frequently in older people. In one study, 61% of patients with Paget's disease reported tinnitus, compared to 36% of healthy patients in the same age group [23]. Paget's disease is not as rare as many people think.
Non-pathological causes
A variety of non-pathological problems can also cause tinnitus. Although the initiating factor can vary, the process usually starts with some initial injury in or around the ear, which may or may not by itself produce tinnitus. Later, the brainstem becomes involved, and tinnitus is produced. Even though the sound and physical sensations appear to be emanating from the ear, researchers believe that the nerve impulses are generated not in the ear itself, but in the dorsal cochlear nucleus (DCN), which is the relay point in the brainstem for acoustic signals. Different types of tinnitus feel and sound distinctively different to the patient. A patient may even experience one type of tinnitus in one ear and another type in the other ear simultaneously. Some of the non-pathological causes of tinnitus are:
- Noise-induced hearing loss
Some researchers believe that noise-induced hearing loss and acoustic trauma are the most common cause of tinnitus in adults [45, 46]. The association between hearing loss and tinnitus is so well-established that anything that causes hearing loss is automatically assumed to cause tinnitus.
Noise-induced hearing loss can be unilateral or bilateral, depending on the source of the noise, and is often accompanied by hyperacusis, which is a lowered tolerance to elevated levels of sound. For example, louder sounds may sound harsh, unpleasant, or screeching. Mild acute noise-induced hearing loss is also accompanied by a feeling of ear fullness. High levels of noise (acoustic trauma) not only kills hair cells in the cochlea, but also kills neurons in the acoustic nerve and the dorsal cochlear nucleus. According to one theory, the automatic repair process in these nerves is the main cause of chronic tinnitus (see Neural Pathways below).
Although conventional audiology tests are still very important in diagnosing noise-induced hearing loss, the otoacoustic emissions test is now considered the definitive test for noise-induced hearing loss. It is particularly valuable for testing the hearing of infants [3].
- Toxic substances
Salicylate, aspirin, ibuprofen and other NSAIDs, wintergreen, antibiotics, cisplatin, quinine, cobalt, sumatriptan, furosemide, hydroxychloroquine, ethacrynic acid, bumetanide, amphotericin B, heavy metals such as mercury, antidepressants such as Wellbutrin (Zyban), and possibly caffeine can cause tinnitus. The inclusion of caffeine in this list is controversial. Salicylates may act by uncoupling oxidative phosphorylation, interfering with the production of ATP. Hair cells are particularly sensitive to low ATP levels. Microcystins, which are hepatotoxins from blue-green algae, have also produced neurological symptoms that include tinnitus [31]. This site has a list of other drugs that can produce tinnitus.
Paradoxically, there are a few reports that indomethacin and other NSAIDs that act as COX-1/lipoxygenase inhibitors also seem to partially protect the ear against noise trauma, at least in mice [40]. Some compounds that mimic glutathione have a similar effect, suggesting that oxidative stress may play a role in noise-induced hearing loss.
Overdoses of hydrocodone, which is usually given with acetaminophen, can cause progressive sensorineural hearing loss leading to deafness, especially in patients with compromised liver function such as from hepatitis C [43]. Patients on hydrocodone/acetaminophen should avoid taking additional over-the-counter pain medication.
Drug-induced tinnitus from triptans and NSAIDs is most often a hissing sound, but ototoxic drugs can also produce a ringing or roaring sound. Drugs can also cause hearing loss, hyperacusis, and "dizziness" that can be mistaken for labyrinthitis. Patients who experience tinnitus after taking a prescription drug are well-advised to ask their doctor whether an alternative is available. Continuing to take an ototoxic drug can result in permanent hearing loss.
- Aging
Aging causes loss of cells that secrete the inhibitory neurotransmitter glycine. Glycine carries the "off" or inhibitory signal from one neuron to another. When glycine-carrying nerve fibers are lost from old age or other factors, the off signal is also lost and certain other neurons begin to fire spontaneously, producing tinnitus. The characteristics of hearing loss caused by aging and by noise trauma are similar.
- Temporomandibular joint (TMJ) syndrome
Although TMJ syndrome is usually associated with clicking and popping noises, the ringing form of tinnitus is also a common occurrence. Whiplash can also cause tinnitus. About 10% of whiplash victims develop some ear problem such as tinnitus, deafness, or vertigo [25]. This might be secondary to TMJ involvement as some have proposed [26,27], or it could be the result of nerve injury or compression.
TMJ syndrome is almost always accompanied by pain or limitation of jaw movement. It's caused by grinding or clenching the teeth by excessive gum chewing, arthritis, or teeth malocclusion. Usually there is a clicking sound when the jaw is opened or closed. It is not unusual for TMJ syndrome to cause muscle spasms that produce tinnitus. Most of the muscle sensory nerves pass close to the nerves that relay sound from your acoustic nerve, so it would not be surprising that pressure on the muscles on the head can trigger tinnitus. It is also very common for movement or pressure on the TMJ to trigger tinnitus. Most experts say that successful treatment of TMJ syndrome will eliminate the tinnitus. However, this does not always happen and even if it does, it may take as long as two years.
According to R.A. Levine, TMJ syndrome is commonly associated with somatic tinnitus. It is generally believed that the ringing noise is caused by the contraction of the jaw muscles and not by the joint itself. If so, the most important thing would be to avoid grinding and clenching the teeth and practice relaxing the affected muscles.
There are several other theories about how TMJ disorders produces tinnitus, including blockage of the Eustachian tube, clonus of the tensor tympani muscle, problems caused by an extra ligament left over from childhood, or impairment of middle ear conduction. The conduction theory is favored by Chole and Parker, and would make sense in cases where TMD is causing a measurable hearing impairment.
Even before painful symptoms appear, TMJ disorders can produce inflammation and cartilage injury that triggers a high-pitched tinnitus (6000 Hz) that is more like a hissing sound than a single tone. In a patient with TMJ syndrome, a single moment of chewing can trigger a sudden onset of tinnitus that lasts for days or weeks. The tinnitus continues until the bad chewing method is corrected.
The most common cause of TMJ is chewing preferentially on one of the mouth or grinding the teeth. Even chewing gum or eating chewy candy can rapidly induce TMJ syndrome. Jaw movements called “chin up” exercises can sometimes reduce TMJ symptoms by strengthening the jaw muscles so they work evenly. These exercises are mainly beneficial if the patient has been chewing unevenly for a long time. In severe cases corticosteroids or even surgery may be prescribed.
- Neck injury and electrocution
Direct blunt neck trauma can cause hearing impairment that resembles noise-induced hearing loss. About 55% of one group of patients who complained of hearing loss after neck trauma also reported tinnitus [28]. There are also reports of hearing loss and tinnitus after high-voltage electric shock and in patients who were struck by lightning. These cases are rare and are poorly understood.
- Middle ear-related causes
Although obstruction of the ear canal by wax (cerumen) is an obvious possible cause of tinnitus, some researchers believe that even small amounts of ear wax may contribute to tinnitus. Conductive deafness caused by perforation of the eardrum is another obvious (and easy to diagnose) factor.
- Dental problems
Dental problems are another possible cause of tinnitus. Tooth abscesses or impacted wisdom teeth can cause tinnitus [34]. In such cases, further dental work will sometimes cure the problem. Other times, the tinnitus gradually becomes fainter over a period of months [35]. One way dental problems can cause tinnitus is by the prolonged neck bending that occurs during dental surgery. Another way is by aggravation of pre-existing TMD. Injury of the nerves during extraction of a wisdom tooth has also been known to cause tinnitus. Another possibility might be inflammation spreading from an infected tooth. There have been cases of bilateral sensorineural hearing loss (which usually causes tinnitus) following dental surgery [36, 37].
- Muscle spasm
Some researchers believe that muscle spasm in head or neck is the most common cause of tinnitus, accounting for as many as 80% of patients [8, 47]. When the noise is made better or worse by changes in bodily posture, or arm or neck movements, the patient has "somatic tinnitus." Somatic tinnitus is usually unilateral. In its earliest stages, it may be caused by hearing trauma, an injury, or a muscle contraction (such as by grinding one's teeth) that compresses some part of the auditory system. Later, cross-talk occurs between the signals the muscles send to the brain and the signals from the ear. For these patients, relaxation therapy and biofeedback, which help the patient establish voluntary control over the muscle, can be helpful. Once alerted to the possibility that stretching and muscle relaxing exercises may be able to alleviate their tinnitus, patients may be able to devise an effective treatment on their own. In extreme cases, botulinum toxin to temporarily paralyze the muscle, or even surgery, can be performed (see Treatment below).
The exercises mainly consist of stretching the facial muscles in the direction away from the ear that is ringing.
For some patients, anything that causes torsion of the neck, such as having bad posture, using a pillow at night, or bending the neck to look through a microscope, even for a few seconds, causes a muscle spasm that invariably produces tinnitus. This muscle spasm and the resulting tinnitus may not occur immediately, but can start several hours after the neck is twisted, making the cause difficult to identify.
Many leading researchers on somatic tinnitus, such as Robert A. Levine [2], believe that somatic tinnitus resulting from muscle spasms is not produced by compression of nerves or blood vessels in the ear as one might suspect, but rather from the convergence in the dorsal cochlear nucleus of sensory signals from muscle spindles in the head and neck with sound signals from the cochlea. This may explain how somatic tinnitus can even occur in deaf people [4]. The characteristics of somatic tinnitus are [5]:
- The muscle and tinnitus are ipsilateral (same side).
- There are no vestibular or neurological abnormalities.
- Tone and speech audiometry is always symmetric and within normal limits.
Therefore, the first step in identifying the cause of tinnitus is to get a hearing test. If hearing is normal, and pathological causes can be ruled out, it points to a possible muscle, dental, or TMJ problem.
The sternocleidomastoid muscle appears to be the culprit in most cases. Palpation of this muscle, which is the large muscle under the ear on both sides of the neck that acts to rotate the head, aggravates tinnitus in many patients. Other muscles that are commonly involved include the masseter, splenius capitis, and even the middle and upper trapezius and temporalis muscles. The lateral pterygoid muscle may also serve as a trigger point. The current thinking is that these effects are mediated by their excitatory connections to the DCN. Palpation or pressure at other points on these same muscles can sometimes reduce tinnitus.
The sources of the muscle sensory signals are proprioceptive (location) and cutaneous (touch) projections. Nociceptive (pain) signals are not involved in tinnitus [6].
- Middle ear infection
A recent Polish study found that over two thirds of the cases of tinnitus in patients below the age of 35 are caused by infection [18]. Infections of the middle ear, which are common in children, are called otitis media. This can be a viral or bacterial infection. The symptoms are otalgia (earache) and temporary sensorineural hearing loss. These patients should avoid swimming activities.
Untreated syphilis can also cause tinnitus and fluctuating hearing loss. About 50% of these otosyphilis patients also experience vertigo (dizziness), which indicates inner ear involvement. Treatment with penicillin and steroids restores hearing only about 25% of the time.
A rare condition known as Ramsay Hunt syndrome can also cause tinnitus. This disease is caused by the varicella zoster virus (VZV), which causes chickenpox and shingles. VZV remains dormant in the nervous system after a patient recovers from chickenpox. Sometimes VZV becomes reactivated and produces a skin rash, called shingles (confusingly named herpes zoster [50, 51]). When the virus affects the 8th cranial nerve and the geniculate ganglion of the facial nerve, VZV causes Ramsay Hunt [52], which is characterized by severe pain behind the ear, tinnitus, facial nerve palsy (sudden paralysis of the face muscles on one side), and a rash on the ear or in the mouth. Ramsay Hunt is similar to Bell's palsy, which is caused by herpes simplex virus. Any paralysis in the face is potentially serious and should be treated as a medical emergency.
Activities such as scuba diving and water skiing can cause traumatic injuries to the ear including eardrum perforation, which causes hearing loss, earache, tinnitus, and vertigo. Sinus infections and migraines are also occasionally associated with tinnitus.
Eustachian tube inflammation can also produce tinnitus, which would usually be accompanied by an earache (otitis) and a sensation of fullness in the ears. This is easily diagnosed by visual examination of the middle ear.
- Over-hydration and dehydration
Hemodialysis patients who become over-hydrated can experience tinnitus along with muscular cramps and other symptoms [30]. Some tinnitus patients report that their symptoms are exacerbated by drinking excess water or soft drinks. In one case, loud, continuous hissing in both ears was eliminated when diet soda was eliminated from the diet.
These causes are not mutually exclusive. Thus, a patient's tinnitus could result from noise-induced hearing loss and an ear infection, or any other combination of causes.
Tinnitus and headache
Many patients with tinnitus also report frequent headaches. Although there are not many articles in the research literature linking tinnitus with either ordinary headaches or migraines, one can imagine several ways the two disorders could be linked.
- Head injuries and muscle spasms resulting from stress can cause both tension headaches and somatic tinnitus.
- Aspirin and other NSAIDs taken for headache can cause toxic tinnitus. Triptans such as sumatriptan (Imitrex) cause tinnitus and occasionally hearing loss.
- Migraines are sometimes associated with tinnitus and vertigo. This more often occurs during the aura phase that precedes the migraine than during the migraine attack itself. The association between tinnitus and migraine aura is probably underreported, because patients are understandably more focused on the intense pain than on the ringing sound. In a recent study, 45% of patients with basilar-type migraine experienced tinnitus during the aura phase [20].
- Intracranial hypotension, which is caused by a leak in the cerebrospinal fluid, causes tinnitus, hearing loss, neck stiffness, vomiting, vertigo and severe headaches that occur suddenly after standing or sitting (orthostatic headache). The symptoms sometimes resemble Ménière syndrome, but intracranial hypotension can also cause “brain sagging” that causes somnolescence, impaired attention, and even coma [19]. This syndrome can also mimic frontotemporal dementia. It is usually caused by lumbar puncture, brain surgery (for instance, to remove a subdural hematoma), or by a fall, or it can occur spontaneously. Intracranial hypotension of unknown etiology is called spontaneous intracranial hypotension or SIH.
- Superficial siderosis A rare condition known as superficial siderosis, or iron in the outer layers of the brain caused by bleeding, causes ataxia and sensorineural hearing impairment which can manifest as tinnitus.
- Subarachnoid hemorrhage Some popular books claim that subarachnoid hemorrhage causes tinnitus. While this may be true, it is not a common cause of tinnitus. Any brain hemorrhage is a medical emergency, and in such cases ringing in the ears may be the least of the patient's problems. The classic symptom of a subarachnoid hemorrhage is a sudden violent headache, usually described as the worst headache of the patient's life.
-
Aneurysms
Brain aneurysms can also cause hearing loss and tinnitus [21]. Tinnitus
resulting from an aneurysm is typically pulsatile with a “swishing” or
roaring sound that coincides with the heartbeat [22].
If you experience this type of tinnitus, especially if it begins suddenly
after a cough, sneeze, or head or neck trauma, or you have other symptoms such
as dizziness, weakness, pain, or ptosis (drooping eyelids), you should have it
checked, because it could be a sign of a weakened blood vessel wall that could
hemorrhage without any warning, possibly causing a stroke. It could also be a
sign of partial occlusion (stenosis) of the carotid artery, or it could be caused
by a harmless malformation of the arteries. Your physician will perform
angiography, ultrasound, or MRA to evaluate it.
In one study, 68% of the patients with pulsatile tinnitus were found to have some underlying pathology, the most common being a dural arteriovenous fistula or a carotid-cavernous sinus fistula [24]. However, in another study, so-called “benign” intracranial hypertension was the most frequent cause.
Neural pathways involved in tinnitus
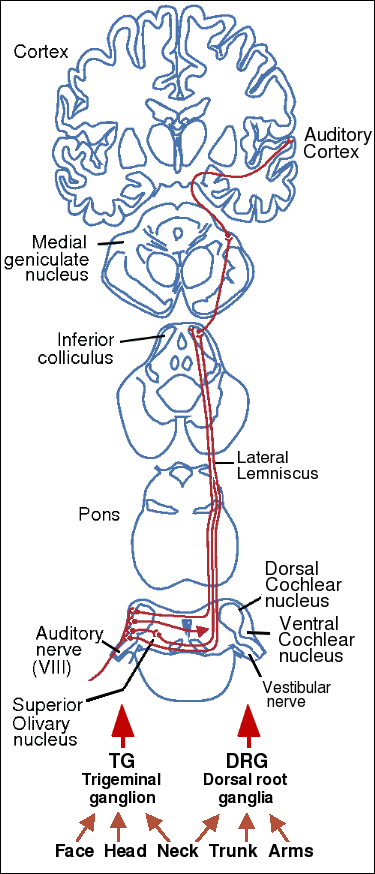 Neural pathways involved in tinnitus. All pathways and nuclei are
bilaterally symmetric.
Neural pathways involved in tinnitus. All pathways and nuclei are
bilaterally symmetric.
Although a variety of factors can cause tinnitus, they all use different parts of the same neural pathways. Therefore, it is important to understand the basic neuroanatomy of the auditory system to understand the various treatments that have been proposed.
Ventral cochlear nucleus
The ventral cochlear nucleus (VCN) is a relay point in the brainstem that
receives data from muscle stretch sensors in the face, head, and neck.
Sensors in muscles of the neck, trunk, and arms send signals to the VCN
by way of the dorsal root ganglia and the trigeminal ganglion. These
sensors tell the brain how strongly the muscle is contracted, and tell
it the position of the body part affected by the muscle. The ventral
and dorsal cochlear nuclei relay signals to each other and to the brain.
Inferior colliculus
The inferior colliculus is an important relay point in the midbrain. It
receives data from lower brainstem nuclei such as the ventral and dorsal
cochlear nuclei, and relays this information to the brain. Neurons in the
inferior colliculus fire more rapidly when tinnitus is occurring. Signals
from the tongue muscle and temporomandibular joint send signals to the
dorsal cochlear nucleus by way of the inferior colliculus. This may explain
why temporomandibular joint syndrome frequently causes tinnitus.
Dorsal cochlear nucleus
The dorsal cochlear nucleus (DCN) is the most important brainstem region
for relaying auditory signals to the brain. It is also the region where
researchers believe the phantom sounds heard by tinnitus sufferers are
generated. As shown in the figure, the dorsal cochlear nucleus receives
auditory signals from the hair cells in the cochlea, where sound is
detected, as well as signals related to eye movements, mediated by the
vestibular system. It also receives a variety of signals from muscle
position sensors in the face, neck, head, trunk, arms, tongue, and
temporomandibular joint, which are relayed to it via dorsal root ganglia
and other nerve centers. The DCN acts as a relay and forwards all these
signals to the appropriate place in the auditory cortex and elsewhere in
the brain. As the signals travel from the DCN to the brain, left and
right are switched. Therefore, sound entering the right ear and muscle
signals on the right side of the head are processed in the left side of
the brain, and vice versa. The feature to remember is that sensory data
from muscles and acoustic data from the ears are both relayed to the
brain at very nearly the same point in the brainstem.
Inhibitory signals
Auditory signals from the cochlea travel to the cochlear nerve, which
combines with the vestibular nerve to form the vestibulocochlear nerve
(acoustic nerve, cranial nerve VIII) on their way to the cochlear nuclei,
which process them and relay them to the brain. However, these signals
are not just 1's and 0's like in a computer. The DCN and VCN process
both "on" (excitatory) and "off" (inhibitory) signals. The inhibitory
signals perform a vital function: they prevent other neurons from getting
stuck in a continuous "on" position. If the inhibitory signals are
blocked due to injury or some other factor, the cochlear nuclei may
"decide" that a sound is present when it is not. The patient would
then hear a ringing or hissing sound.
These inhibitory signals are carried by the neurotransmitter glycine. This means that specific neurons, called glycine interneurons, transmit "off" signals to other neurons, which contain receptors for glycine. If a glycine neuron is injured and dies, the cells it is connected to must adapt to the loss. Each neuron "grieves" in its own way. Some neurons adapt by decreasing the number of glycine receptors, while other adapt by increasing the number of receptors. Thus, the entire network is affected and may start sending false signals. Some researchers believe that inhibitory synapses are more fragile than excitatory synapses. If so, that could explain why even small injuries to the head can cause lifelong tinnitus.
Because the cochlear nuclei are so important in tinnitus, it is sometimes said that tinnitus is primarily a brain phenomenon. Proof of this is that tinnitus can still occur after the auditory nerve has been cut. About 50% of these patients, who are now completely deaf, still experience tinnitus. Thus, even those people so tormented by tinnitus that they would prefer permanent deafness cannot always obtain relief.
However, calling tinnitus a "brain disorder" would be misleading. Tinnitus does not begin in the auditory cortex [7], although some researchers believe that tonotopic remapping (functional rewiring of the cortex) can occur on the auditory cortex. In this sense, tinnitus has some similarities to phantom limb syndrome. Tinnitus is not, however, a brain disease, and it is most definitely not a symptom of a psychiatric disorder or hysteria. In the absence of normal stimuli, the DCN undergoes synaptic plasticity, a form of neuronal reorganization similar to learning that, according to the current theory, results in tinnitus.
Synaptic plasticity
Trauma from loud noises not only injures the hair cells in the
cochlea; it also causes neurodegeneration, or death of nerve
cells, in the auditory nerve and brainstem. Researchers have found
that in rodents, noise trauma causes neurodegeneration in the dorsal
cochlear nucleus that continues to progress for
up to two weeks, as well as neurodegeneration in the auditory nerve
and ventral cochlear nucleus that can continue to progress for
up to eight months after sound exposure.
The exact length of time that neurodegeneration continues in humans
is not known, but is probably similar.
This neurodegeneration in turn triggers an automatic
repair process that includes sprouting and regrowth of new axons
and nerve terminals. Although they try to reconnect in exactly the
same way as before, the new nerve terminals are not always able to
do so; some rewiring, called synaptic plasticity, occurs.
As the neurons repair and regrow, two things can happen. First, since there are fewer inhibitory glycine neurons, the neurons may begin sending continuous signals to the brain. Secondly, signals from other, non-acoustic sources, such as the temporomandibular joint or muscle sensors in the head and neck, may get mixed with sound signals in such a way that movement of these muscles can trigger the generation of phantom sounds.
In some ways, this is bad news. We cannot administer drugs that interfere with synaptic plasticity, because it is essential for both learning and repair within the nervous system. Synaptic plasticity is an essential part of how we remember things. On the other hand, it is good news: it means these synapses may, in principle, be able to "learn" not to generate false signals. Researchers have found that this is indeed possible. White noise therapy (see below) can "teach" these neurons not to produce the false signals. If white noise is given in time, and for a long enough period, tinnitus can be prevented (see Sound therapy below).
Anxiety
Physicians used to believe that tinnitus results from anxiety or stress. We now know that this is false. Animal studies have conclusively shown that anxiety does not cause tinnitus. However, tinnitus often provokes anxiety and creates stress, because patients fear they may be losing their hearing or may have a serious underlying problem. Anxiety may exacerbate the tinnitus and the distress felt by patients. Patients with a "perfectionistic" personality type may be more likely to seek treatment, leading to the inaccurate perception among physicians that tinnitus has a psychological component. Tinnitus is also not a conditioned reflex, but different patients may be more or less disturbed by the same amount of tinnitus.
Treatment
Once mechanical problems such as impacted wax are eliminated as possible causes, a hearing test should be given to determine whether you have noise-induced hearing loss. Most treatments are still in the experimental stage. The most promising areas of research at the moment are sound therapy, neck exercises, and acupuncture. Some progress is also being made using drugs to inhibit the neuronal pathways.
If the tinnitus is intermittent, this is generally a good sign, because it is proof that the auditory system is capable of functioning normally. Finding the trigger is then a matter of deduction from what is different in the minutes and hours before the tinnitus starts. However, even continuous tinnitus resulting from trauma or partial hearing loss is not necessarily untreatable, because it could be mixed with a treatable component.
Drugs
There are currently no drugs approved for treatment of tinnitus. The drugs listed below are in various stages of experimental testing.
Lidocaine The earliest treatment ever discovered was lidocaine (Xylocaine), which effectively suppresses tinnitus. Lidocaine is a local anesthetic which acts by blocking voltage-gated sodium channels in neurons, preventing neuronal transmission. Since it is only short-acting (hours) and must be injected by a physician, it is not considered to be useful as a treatment. High doses of lidocaine can also cause tinnitus. Intradermal lidocaine is a possibility, but it has not been studied thoroughly.
Glycine receptor agonists For tinnitus that is caused by overexcitation of the cochlear nucleus, it may be possible to develop glycine receptor agonists. These drugs would mimic the natural neurotransmitter glycine, and re-balance the excitation / inhibition pathways. Thus, the future for tinnitus sufferers is not as gloomy as is commonly believed. Research into glycine receptor agonists is underway.
An interesting fact is that the poisonous alkaloid strychnine is a glycine receptor antagonist, and acts by blocking the glycine receptor; thus, glycine receptor agonists might also be beneficial as a treatment for strychnine poisoning.
GABA-A receptor agonists GABA is another inhibitory neurotransmitter, similar to glycine. A class of drugs called benzodiazepines already exists. These drugs are GABA-A receptor agonists, and might be expected to work on tinnitus by activating the inhibitory limb of the neural network. Some researchers have reported moderate success in treating tinnitus with GABA agonists such as baclofen, clonazepam, and diazepam. However, these drugs are also tranquilizers, and cause undesirable CNS side effects. If the current theory about tinnitus being generated in the brainstem is correct, topical application of these drugs is not likely to work, because the drug would be unable to reach the brainstem. Thus, a systemic drug that is targeted to the brainstem is needed.
There is one report that a high dose of taurine, a partial agonist of glycine and GABA receptors, attenutates tinnitus in rats by decreasing noise in the auditory pathway [38].
Midazolam One report out of Germany reported partial protection by midazolam, another benzodiazepine with GABA(A) modulating properties that is used as a sedative and anticonvulsant. Midazolam was given to rats experiencing salicylate-induced tinnitus [39], which is a commonly used experimental model for tinnitus. Benzodiazepines can cause anterograde amnesia and long-lasting memory problems.
Anticonvulsants Because of the parallels between tinnitus and epilepsy (both of which result from overexcitation of neurons), low doses of anticonvulsants such as gabapentin and carbamazepine have been tried, but with little success so far. Although gabapentin acts on the GABA pathway, it is not a direct GABA agonist; it is believed to work by activating glutamic acid decarboxylase, the enzyme that converts glutamate to GABA. It therefore acts by causing the cell to produce more of the inhibitory neurotransmitter GABA.
Acamprosate Acamprosate, a drug used to treat alcoholism, acts as a glutamate antagonist and GABA agonist. It acts by increasing the number of GABA reuptake sites and increasing GABA transmission. One Brazilian group reported a modest but statistically significant benefit using acamprosate to treat tinnitus.
NMDA antagonists A class of drugs known as NMDA receptor antagonists has been shown to block salicylate-induced tinnitus in animals. These drugs interfere with the excitatory neurotransmitter glutamate. However, salicylate may produce tinnitus by a different mechanism than normal tinnitus, so NMDA antagonists may not be effective in patients. Since glutamate is the predominant neurotransmitter in the brain, these drugs would also act as general tranquilizers or anesthetics. Also, some NMDA antagonists are potent neurotoxins. NMDA antagonists such as caroverine have had moderate success, but unfortunately this class of drugs has very significant side effects, such as psychosis. The anti-Alzheimer drug memantine, and neramexane, which are both NMDA receptor antagonists, are currently being tested.
Neuromuscular-blocking drugs The only neuromuscular blocking drug currently used for tinnitus is botulinum toxin, which has been used to paralyze specific muscles. Other drugs, such as dantrolene, a muscle relaxant used to treat muscle spasticity, and drugs similar to tubocurarine, a powerful quaternary ammonium muscle relaxant, have not been tested. Some antihistamines, such as orphenadrine, which is used to treat muscle spasms, might also be useful. However, there are few reports of these drugs being tested. Injection of botulinum toxin into a muscle will paralyze it for 4-6 months; therefore, injecting it into one of the large muscles needed for chewing or supporting the head would be a very bad idea.
Antidepressants Tricyclic antidepressants such as nortriptyline and serotonin reuptake inhibitors such as paroxetine and sertraline have been reported to reduce tinnitus. These drugs may work because of similarities between tinnitus and neuropathic pain. However, clinical studies have shown conflicting results, with tinnitus sometimes being reduced in depressed patients but not non-depressed patients.
Hyperbaric oxygen The outer hair cells in the organ of Corti facilitate the sensory response of the inner hair cells. The inner hair cells, which are connected to nerve fibers, are the primary sensors for sound. Inner and outer hair cells have no direct blood supply. When a loud sound is heard, they become very active and can deplete their limited supplies of oxygen and their energy molecule, ATP. Thus, it has been hypothesized that hyperbaric oxygen could be beneficial in cases of noise-induced hearing loss and acoustic trauma if it is administered soon enough. However, so far the research has been inconclusive. Beneficial results are sometimes seen if it is administered within the first few months [44]. A similar theory has been proposed for magnesium (see below). If these theories are correct, they would predict that oxygen and magnesium would be most effective within a few hours of a noise trauma, and become much less effective as time goes on.
Several chapters on drug treatments can be found in reference [12].
Sound therapy
White noise The theory that tinnitus is created by the loss of inhibitory stimuli has resulted in the most promising new therapy for tinnitus so far: white noise therapy. White noise, such as that produced by a radio tuned to an empty frequency or a sound generator like a Marsona, has two effects: first, it masks the ringing sound; and second, it helps to stimulate the inhibitory pathways by producing a continuous background of sound. The extent to which these pathways can be rewired is still not entirely clear, but it is clear that white noise creates additional excitatory and inhibitory stimuli that appear to be able to influence the synaptic regrowth in the DCN, and prevent tinnitus from starting. (They are also great for preventing insanity caused by having a neighbor who is overly fond of rock music.)
According to the theory described above, noise-induced hearing loss produces tinnitus because it is, in effect, creating silence. Indeed, most normal people will experience tinnitus when placed in an anechoic chamber. Therefore, one could logically expect background noise to prevent it. However, this is difficult to prove, because noise also masks tinnitus.
Nevertheless, it is true--at least in animals. Noreña and Eggermont have found that if white or blue noise (5kHz-20kHz) is presented immediately after noise trauma and maintained over a period of several weeks, the neuronal changes that cause tinnitus and hearing loss are abolished [9, 10]. This remarkable finding shows that it may be possible to prevent noise-induced tinnitus even in cases of acoustic trauma.
It goes without saying that white noise, or any other noise, above 85 decibels will cause hearing loss, especially if maintained for long periods of time. Moreover, there is some suggestion that white noise could be harmful for infants. Also, it stands to reason that sound therapy, or any other therapy, will not work unless whatever caused the tinnitus in the first place is stopped.
The theory would predict that for a maximal effect, a sound generator would have to be running continuously, not just when the patient's ears are ringing. Also, the closer the frequency of the generated sound to the frequency of the tinnitus, the more effective it should be.
Update, Oct. 24, 2024 For ringing-type tinnitus this sometimes works: if you play a note on a piano the exact pitch of the ringing, the ringing will stop. It has to be exact, not an octave above or below. Sometimes the ringing will start up again at a different pitch, e.g. D-flat instead of E-flat. It might not be as effective if it's ringing at two frequencies at once. It has no effect on hissing-type tinnitus.
Stimulation of muscle stretch receptors
Certain neck exercises have also been highly effective at eliminating tinnitus in some cases of somatic tinnitus. Specific exercises are sometimes recommended to stretch the sternocleidomastoid muscle. For example, the patient may be instructed to lower the shoulders, tilt the head up, then pull in the jaw to relax the muscle. This is an easy and safe therapy if done within reason. Another exercise that sometimes works is to rotate the head in the direction away from the ear that is ringing while simultaneously pulling the lips in the same direction. The theory predicts that relaxing the muscle will reduce the stretch receptor signal and thereby reduce the excitatory stimulation to the dorsal cochlear nucleus that creates the tinnitus. If the correct muscle is stretched, the tinnitus will often disappear within a few seconds. If the patient is unable to stretch the correct muscle, but makes an effort to relax the muscles around the ear, it may take longer for the noise to disappear. Neck exercises need to be tailored to the individual. They are less likely to work if the tinnitus is caused by some factor other than muscle spasm.
Surgery and electrical stimulation
Microvascular decompression A surgical technique called microvascular decompression, which is an effective treatment for trigeminal neuralgia, is sometimes beneficial for tinnitus as well. What happens is that a blood vessel, usually an artery, compresses the cochlear nerve, causing tinnitus and vertigo. If this is fixed within about four years, recovery is sometimes possible [48]. More drastic treatments include cochlear implants that replace the missing neuronal stimulation with artificial electrical signals. Surgery of the ear or brain is extremely dangerous, and is considered a treatment of last resort.
Meniere's disease For Ménière's disease, an experimental treatment involves intratympanic injections of drugs such as gentamicin or steroids. In this procedure, the eardrum is anesthetized and the drug is injected through the eardrum. Since this procedure perforates the eardrum, it is difficult to evaluate its effectiveness for tinnitus. Because of the extreme invasiveness of this procedure, patients are understandably reluctant to undergo it. Patients might also falsely report improvement in order to avoid a second treatment.
Cochlear implants Because hearing loss produces tinnitus, anything that even partially restores hearing will often reduce the tinnitus. Many studies have shown that, if a cochlear implant restores some hearing, it usually reduces the tinnitus. However, because a cochlear implant completely and permanently destroys all remaining normal hearing, only patients with profound hearing loss are candidates for a cochlear implant. A neurologist should be the one to do a referral.
In a recent study, all the patients with tinnitus reported a partial (61%) or complete (39%) elimination of their tinnitus after receiving a cochlear implant. A cochlear implant produced tinnitus in 12% of the patients who did not have it before the operation [17].
Hearing aids A hearing aid may have the same effect, and would be much safer than an implant. There are special hearing aids that contain sound generators which stimulate the auditory pathway. In some patients, the combination of restored hearing and sound therapy can cause the neural pathways to reorganize in such a way that the generation of tinnitus is reduced. Unfortunately, as with implants, if hearing cannot be restored, sound therapy is unlikely to work.
Electrical brain stimulation Some researchers believe that another treatment called deep brain stimulation might be able to treat tinnitus. Magnetic stimulation, which is a non-invasive procedure, is used to find the precise location where tinnitus is being perceived on the auditory cortex. Then a permanent electrode is inserted at this location to prevent the patient from hearing the noise. This treatment will not restore hearing. It is still in the experimental stages and is not available for patients yet.
Another new technique involves electrical stimulation of the auditory cortex. This is based on a new theory that in tinnitus, there are too many neurons on the auditory cortex that respond to a particular sound frequency. It has been shown that direct electrical stimulation of the auditory cortex can block tinnitus and partially restore hearing thresholds [42]. The technique is still highly experimental and there is still a large variability in the results.
To get around the risks of stimulating the brain directly, one group of researchers stimulated the vagus nerve in rats with tinnitus and paired it with a loud sound stimulus [41]. Only the left vagus nerve was used to minimize cardiac complications. Repeating the pairing up to 6,000 times alters the frequency map of sound represented on the auditory cortex, degrading the frequency tuning of the individual brain neurons and normalizing the brain's response to sound. The researchers found that this procedure, which requires surgery, reduced tinnitus in rats for at least three weeks. Although it was impossible to be certain the rats were really experiencing tinnitus, gap detection tests of their hearing showed changes consistent with a long-lasting reduction of tinnitus.
Transcutaneous electrical nerve stimulation A related treatment is transcutaneous electrical nerve stimulation (TENS), a treatment sometimes used for chronic pain. The theory is that electrical stimulation will activate the dorsal cochlear nucleus, increasing its ability to inhibit somatic tinnitus. In a recent study [32], 43 out of 240 patients (17.9%) with somatic tinnitus reported an improvement. In another study in Spain involving 26 patients, 23% reported partial improvement and 23% reported complete improvement [33]. Although these results were statistically significant, some have suggested that they could result from a placebo effect. There is still doubt over the efficacy of TENS for tinnitus.
This treatment should not be confused with electrical stimulation of the ear, which was proposed as a treatment back in the 1980s. If this treatment worked at all, it was likely due to its effects on the muscle or by changing blood circulation.
Alternative medicines and nutritional supplements
Alternative medicine treatments, including ginkgo biloba, zinc, magnesium, and magnets, in general are believed by the medical establishment to have little benefit, but saying even this is controversial, because little solid research has been done on many of these treatments. However, there is no doubt that good general nutrition is important for recovery from any type of injury, including injury that produces tinnitus.
Magnesium is a very promising new treatment for noise-induced hearing loss [13, 14], which often causes tinnitus, but in such cases therapy must start within a few hours of the noise trauma to be effective.
Ginkgo biloba is supposed to act as a vasodilator, and may improve blood circulation in regions near the cochlea that have been stressed by noise trauma, but so far there has been more enthusiasm than rigorous science in the field.
Dihuang 地黄 (Rehmannia glutinosa) is a Chinese herb traditionally used for tinnitus and to protect against noise-induced hearing loss. Some evidence suggests it may induce GDNF (glial cell line-derived neurotrophic factor) or act as an antioxidant. It has not been rigorously tested.
Vinpocetine (Cavinton) Vinpocetine is an anti-inflammatory agent that inhibits the enzyme IKK. A recent report suggests it may be useful in treating chronic obstructive pulmonary disease. One Polish group in 1997 [29] reported improvement in hearing and tinnitus caused by acoustic trauma if given within the first week, when inflammation was presumably at a maximum. However, there have been no reports since then. There are anecdotal reports that it may also act as a vasodilator.
Zinc There is wide variability in the reported results with zinc. Some studies on the benefits of zinc have been hampered by researchers giving metallic elemental zinc instead of the active form, which is Zn2+. There is also wide variation in epidemiological results on the prevalence of zinc deficiency, with estimates ranging from 2 to 69% of the population. As we scientists say, more research is needed.
Acupuncture has produced dramatic success in cases of somatic tinnitus that were not accompanied by hearing loss [11]. Other researchers have had less positive results. Because many Westerners seriously underestimate the complexity of acupuncture and the amount of skill necessary to make it work, it is necessary to find an acupuncturist experienced in tinnitus treatment.
Magnets appear to be useless, but magnets should not be confused with transcranial magnetic stimulation, which is an accepted technique for inducing electrical currents in the brain noninvasively. Electrical stimulation of the scalp and auricle has produced beneficial results in a few people.
Cognitive behavior therapy
Cognitive behavior therapy is the new term for psychotherapy, which has acquired very negative connotations. Since tinnitus is a physical problem, there is little reason to expect a benefit from cognitive behavior or "talk" therapy. The main goal seems to be to get the patients to ignore the sounds and live with it: to learn, in effect, to stop worrying and love their tinnitus. Relaxation therapy, however, may be of benefit in reducing muscle tension that contributes to tinnitus.
Update: Recent findings on tinnitus
Although patients might disagree, a few researchers believe that tinnitus can be a signal of inner ear repair. In one study patients with sensorineural hearing loss who were in the “tinnitus-often” group had a much higher frequency of hearing improvement rate than “tinnitus-rare” patients [49]. The authors suggested that hearing loss without tinnitus is fundamentally different than hearing loss with tinnitus. However, not all researchers agree with this finding.
More researchers are being converted to the new theory that the noise heard in tinnitus is actually created in the auditory cortex, not the brainstem. The theory is that some hyperexcitation is going on in the brain that generates tinnitus. If true, then transcranial magnetic stimulation of the auditory cortex might help to induce synaptic reorganization and reduce it. Much more work needs to be done to find out if this is a viable treatment.
Update: Benefits from transcranial magnetic stimulation questioned
Repetitive transcranial magnetic stimulation (rTMS) is a way of using powerful magnetic fields to induce neuroplastic effects in the brain. The theory is that tinnitus is like phantom limb syndrome, where the patient feels pain in a limb that is no longer present. It's believed that phantom limb syndrome is caused by plastic changes in the brain, i.e. neurons forming synapses in the wrong place. If so, then inducing more neuroplastic changes should give the brain a chance to correct itself.
So far the results have been mixed. Nordmann et al. [53] reviewed 29 studies of rTMS and concluded “Our results do not suggest that there are systematic alterations of cortical excitability changes during rTMS treatment.” Another meta-analysis [54] found that there was some benefit but a high variability of studies design and reported outcomes.
This might mean we don't know the best way to use rTMS; maybe a combination of TMS and acoustic stimulation would work better. But it could also mean that the analogy with phantom limb syndrome is a red herring. Patients, after all, often report that tinnitus comes and goes, suggesting that the cause of the problem may lie elsewhere, such as the auditory nerve. If so, we would only be treating the symptoms. But I suspect for many patients that would be good enough.
Update: Possible breakthrough in preventing noise-induced hearing loss (July 13, 2016)
Hill, Yuan, Wang, and Sha reported today in the Journal of Neuroscience that noise-induced hearing loss of hair cells is mediated in mice by an enzyme called AMP-activated protein kinase. If this finding holds up, and if it works in humans, it means that it might be possible to develop a drug that can protect against hearing loss and the tinnitus that accompanies it.
References
[1] Tinnitus: Pathology and Treatment, Langguth et al, eds. Progress in
Brain Research vol. 166 (2007).
[2] Tinnitus: Theory and Management J. B. Snow, ed. (2004)
[3] Handbook of Otoacoustic Emissions (A Singular Audiology Text) (Paperback)
by James W. Hall (Author)Singular; 1st edition
[4] Exp Brain Res. 2003 Dec;153(4):643-8. Epub 2003 Nov 5.
CNS somatosensory-auditory interactions elicit or modulate tinnitus.
Levine RA, Abel M, Cheng H.
[5]Am J Otolaryngol. 1999 Nov-Dec;20(6):351-62.
Somatic (craniocervical) tinnitus and the dorsal cochlear nucleus hypothesis.
Levine RA.
[6] Prog Brain Res. 2007;166:107-23.
Neural mechanisms underlying somatic tinnitus.
Shore S, Zhou J, Koehler S.
[7] Ref. 1, page 20
[8] Ref. 1, page 22
[9] Noreña AJ, Eggermont JJ.
Enriched acoustic environment after noise trauma reduces hearing loss
and prevents cortical map reorganization.
J Neurosci. 2005 Jan 19;25(3):699-705.
[10] Noreña AJ, Eggermont JJ.
Enriched acoustic environment after noise trauma abolishes neural
signs of tinnitus.
Neuroreport. 2006 Apr 24;17(6):559-63.
[11] Ref. 1 page 202
[12] Ref. 1 page 249-338
[13] J. Attias, S. Sapir, I. Bresloff, I. Reshef-Haran, and H. Ising (2004).
Clin. Otolaryngol. 29, 635-641.
[14] J. Attias, G. Weisz, S. Almog, A. Shahar, M. Wiener, Z. Joachims,
A. Netzer, H. Ising, E. Rebentisch, and T. Guenther (1994).
Am. J. Otolaryngol. 15, 26-32.
[15] Principles of Neurology, 8th ed. , Ropper and Brown, eds., p 252.
[16]. Kiang NY, Moxon EC, Levine RA. Auditory nerve activity in cats with
normal and abnormal cochleas. Ciba Found Symp 1970:241-268.
[17]. Pan T, Tyler RS, Ji H, Coelho C, Gehringer AK, Gogel SA. Am J Audiol. 2009 Dec;18(2):144-51.
[18]. Raj-Koziak D, Bartnik G, Skarzyński H, Piłka A, Fabijańska A, Borawska B.
Otolaryngol Pol. 2008;62(4):476-9.
[19]. Gordon, N. Spontaneous intracranial hypotension.
Dev Med Child Neurol 2009:51(12)932-5.
[20]. Basilar-type migraine: clinical, epidemiologic, and genetic features.Neurology.
Kirchmann M, Thomsen LL, Olesen J. 2006 Mar 28;66(6):880-6.
[21]. Novel surgical treatment of a transverse-sigmoid sinus aneurysm presenting as pulsatile tinnitus:
technical case report. Gologorsky Y, Meyer SA, Post AF, Winn HR, Patel AB, Bederson JB.
Neurosurgery. 2009 Feb;64(2):E393-4; discussion E394.
[22]. Pulsatile tinnitus: a harbinger of a greater ill? Liess BD, Lollar KW, Christiansen SG, Vaslow D.
Head Neck. 2009 Feb;31(2):269-73.
[23]. Tinnitus and Paget's disease of bone. Mackenzie I, Young C, Fraser WD.
J Laryngol Otol. 2006 Nov;120(11):899-902.
[24]. Pulsatile tinnitus--a review of 84 patients. Waldvogel D, Mattle HP, Sturzenegger M, Schroth G.
J Neurol. 1998 Mar;245(3):137-42.
[25]. Int Tinnitus J. 2002;8(2):129-31.
Temporomandibular joint dysfunction in whiplash injuries: association with tinnitus and vertigo.
Boniver R
[26]. A review of the otological aspects of whiplash injury.
Tranter RM, Graham JR.
J Forensic Legal Med. 2009 Feb;16(2):53-5. Epub 2008 Nov 1
[27]. Tinnitus in Whiplash Injury.
Claussen C, Constantinescu L.
Int Tinnitus J. 1995;1(2):105-114.
[28]. Hearing loss after direct blunt neck trauma.
Segal S, Eviatar E, Berenholz L, Vaiman M, Kessler A, Shlamkovitch N.
Otol Neurotol. 2003 Sep;24(5):734-7.
[29]. [Treatment results of acoustic trauma]
Konopka W, Zalewski P, Olszewski J, Olszewska-Ziaber A, Pietkiewicz P.
Otolaryngol Pol. 1997;51 Suppl 25:281-4. Polish.
[30]. Clinical events occurrence and the changes of quality of life in chronic
haemodialysis patients with dry weight determined by echocardiographic method.
Chang ST, Chen CL, Chen CC, Hung KC.
Int J Clin Pract. 2004 Dec;58(12):1101-7.
[31]. Fatal microcystin intoxication in haemodialysis unit in Caruaru, Brazil.
Pouria S, de Andrade A, Barbosa J, Cavalcanti RL, Barreto VT, Ward CJ, Preiser W,
Poon GK, Neild GH, Codd GA. Lancet. 1998 Jul 4;352(9121):21-6.
[32].Transcutaneous electrical nerve stimulation (TENS) of upper cervical
nerve (C2) for the treatment of somatic tinnitus.
Vanneste S, Plazier M, Van de Heyning P, De Ridder D.
Exp Brain Res. 2010 Jul;204(2):283-7.
[33]. Trans-electrical nerve stimulation (TENS) for somatic tinnitus.
Herraiz C, Toledano A, Diges I.
Prog Brain Res. 2007;166:389-94.
[34] Ref. 2, page 115.
[35] Ref. 2, page 117.
[36]. Bilateral idiopathic sensorineural hearing loss following dental surgery.
Wilson RH, Witkowski CE, Wilson AA.
J Am Acad Audiol. 2009 Mar;20(3):180-6.
[37]. Acute sensorineural hearing loss immediately following a local anaesthetic dental procedure.
Tan TS, Shoeb M, Winter S, Frampton MC.
Eur Arch Otorhinolaryngol. 2007 Jan;264(1):99-102. Epub 2006 Aug 1
[38]. The effect of supplemental dietary Taurine on Tinnitus and auditory discrimination in an animal model.
Brozoski TJ, Caspary DM, Bauer CA, Richardson BD.
Hear Res. 2010 Sep 22
[39]. Midazolam reverses salicylate-induced changes in brain-derived neurotrophic
factor and arg3.1 expression: implications for tinnitus perception and auditory
plasticity. Panford-Walsh R, Singer W, Rüttiger L, Hadjab S, Tan J, Geisler HS,
Zimmermann U, Köpschall I, Rohbock K, Vieljans A, Oestreicher E, Knipper M.
Mol Pharmacol. 2008 Sep;74(3):595-604.
[40]. The non-steroidal anti-inflammatory drugs protect mouse cochlea against
acoustic injury. Hoshino T, Tabuchi K, Hirose Y, Uemaetomari I, Murashita H,
Tobita T, Hara A. Tohoku J Exp Med. 2008 Sep;216(1):53-9.
[41].
Engineer ND, Riley JR, Seale JD, Vrana WA, Shetake JA, Sudanagunta SP, Borland MS, Kilgard MP.
Reversing pathological neural activity using targeted plasticity. Nature 2011, Jan. 12.
[42]. Zhang J, Zhang Y, Zhang X. Auditory Cortex Electrical Stimulation Suppresses
Tinnitus in Rats. J Assoc Res Otolaryngol. 2010 Nov 6
[43]. Profound hearing loss associated with hydrocodone/acetaminophen abuse.
Friedman RA, House JW, Luxford WM, Gherini S, Mills D. Am J Otol. 2000 Mar;21(2):188-91.
[44]. J Spec Oper Med. 2009 Summer;9(3):33-43. Tinnitus, a military epidemic: is
hyperbaric oxygen therapy the answer? Baldwin TM.
[45]. Axelsson, A; Prasher, D. (2000). Tinnitus induced by occupational
and leisure noise. Noise & Health: A Quarterly
Inter-disciplinary International Journal; 2(8): 47-54.
[46]. Humes, LE, Joellenbeck, LM, Durch, JS (2006). Noise and
military service: Implications for hearing loss and tinnitus.
Washington D.C.: The National Academies Press.
[47]. This does not necessarily conflict with the earlier claim that
noise-induced hearing loss is the most frequent cause of tinnitus. It could be, as
described in the section on Neural Pathways, that a combination of events
is responsible.
[48]. Neurosurgery. 2010 Apr;66(4):656-60. Microvascular decompression for tinnitus:
significant improvement for tinnitus intensity without improvement for distress.
A 4-year limit. De Ridder D, Vanneste S, Adriaenssens I, Lee AP, Plazier M, Menovsky T,
van der Loo E, Van de Heyning P, Moller A.
[49].Hikita-Watanabe N, Kitahara T, Horii A, Kawashima T, Doi K, Okumura S. (2010).
Tinnitus as a prognostic factor of sudden deafness.
Acta Otolaryngol. 2010;130(1):79-83
[50]. Fundamental Virology, 3rd ed., Fields, Knipe, and Howley, eds, p. 220.
[51]. Medical Virology, 4rd ed., White, Fenner, eds. p. 153.
[52]. Sweeney, CJ, Gilden, DH (2001) Ramsay Hunt Syndrome. J. Neurol. Neurosurg.
Psychiatry 71(2), 149-154.
[53]. Nordmann G, Azorina V, Langguth B, Schecklmann M.
A systematic review of non-motor rTMS induced motor cortex plasticity.
Front Hum Neurosci. 2015 Jul 21;9:416.
[54]. Soleimani R, Jalali MM, Hasandokht T.
Therapeutic impact of repetitive transcranial magnetic stimulation (rTMS) on
tinnitus: a systematic review and meta-analysis.
Eur Arch Otorhinolaryngol. 2015 May 13.
Comments
30 Mar 2010, 21:32
06 Apr 2010, 08:46
18 Apr 2010, 17:43
Thank You
19 Apr 2010, 08:39
19 Apr 2010, 10:02
19 May 2010, 20:58
I have been struggling with catastrophic tinnitus for about five months now. Recently, I discovered the somatic component involved in changing the intensity of the tinnitus. In 2007 it was discovered that I have some old injuries to the first and second cervical vertebrae that have bone spurs and protruding disc damage. (Injuries may be due to a combination of football, skydiving, whiplash and falls) Do you know of research to suggest this as a possible cause and concommitent surgical aleviation of the tinnitus through removal of the spurs and repair of the disc??? I appreciate your kind consideration in this matter.
JED
20 May 2010, 02:16
21 May 2010, 08:49
21 May 2010, 09:05
22 May 2010, 06:50
25 May 2010, 18:02
29 May 2010, 12:49
29 May 2010, 22:06
05 Jun 2010, 01:18
08 Jun 2010, 15:30
I hope you find something that helps you because this can be such a difficult thing to live with. Good luck to all of you!
10 Jun 2010, 21:54
Or is this idea pure fiction?
Very good article by the way.
11 Jun 2010, 09:28
16 Jun 2010, 20:25
You may wonder how I found out it was 6450hz. I am a retired electronics tech so went looking for a noise generator for my computer. I installed it and then started to play with a single channel and raised the noise in headset plugged into the computer until the noise in my head equaled the noise in the headset.
Whats the advantage?
Well if you know what frequency your tinntius is vibrating at, you may find using this generator with multiple tones then recording it and playing it back at night may help.
Because my tinnitus is now out of the audible range, I can use a white noise generator now, When it was 6450hz I just mucked around with something until it worked for me. Everyone will be different.
I have a bad back injured in 1989 and have always used Chiropractors to get me through the tough parts. This is what I have found so far.
Any massage or stretching of the Sternocleidomastoid muscles causes me more tinnitus the next few days after the massage or stretching is done. I see no improvement and go through a tough patch afterwards for no improvement. So I know longer massage manually.
I started to get a "full in the head feeling" very similar to be all stuffed up with a cold and bad headaches. When I did, I went to my chiropractor and had a head manipulation. Within 48 hours the head pressure and headaches were gone. This works for me, everyone is different.
After a manipulation, the tinnitus goes much higher, my normal tinnitus is a 2 out of 5, after manipulation its a bad 4 out of 5. Two days later I am back to a 2 and "sometimes" it will almost disappear.
Each time I am manipulated the frequency rises. So I have gone from 6450hz to something I can no longer hear with my ears. It would be a sound that is similar to a jet sitting on a runway, the highest pitch you can remember is what I hear.
This believe it or not is "good news" for me, because I found tinnitus in the regular audio spectrum, the spectrum of the human voice more irritating. So a 4out 5 at a very high frequency is far less irritating then a 4 out of 5 at a human voice level, for me.
Last thing I have found that helps if you have neck tinnitus is a hand shower that has a pulsating shower setting. I sit in the shower every night before bed and crank the hot water up to the highest I can tolerate. I then use the hand shower on pulse, and go up and down the Sternocleidomastoid muscles on both sides of my neck and across the back of my neck. I do this for as long as I can possibly tolerate it. About 5 minutes or so.
I find that it reduces the tinnitus amplitude by "1" when I am going to sleep. I do the same thing in the morning and, if I have too, I do it mid day, I do.
Cold water or cold ice packs cause things to get worse for me. Hot packs do nothing. No idea why but only pulsating water works.
Thanks for this site. I have tried most of the remedies mentioned and none work so thought I would add a few of my own. Perhaps some of these things will help others.
This is a classic description of somatic tinnitus: the patient's neck is bent or twisted for a long period of time. During this period, tinnitus occurs, and the patient, believing the sound to be harmless, ignores it. Subsequently the sound occurs spontaneously, and it becomes more and more disturbing until, often years later, the patient finally seeks medical advice. By this time, the original cause has often been forgotten.
